Women and Aging: Equity in the Wellbeing of Older Adults in Central Indiana
A persistent socioeconomic gap between men and women has implications for their relative wellbeing as they age into retirement and beyond. Socioeconomic inequities established in adulthood carry over into old age. Women often require more assistance as they age yet face financial disadvantages that discourage them from seeking the care they need. This report explores the gender inequities that may contribute to disparities in physical, mental, and cognitive well-being and implications for long-term care needs.
Key Findings
-
Socio-Economic Inequities: Women often enter retirement with lower incomes and fewer assets compared to men. Contributing factors include lower lifetime earnings and a higher likelihood of living alone. In Central Indiana, older women (age 65 and over) on average have less than 60 percent of the personal income of older men.
-
Racial Disparities Among Older Women: Among older women (age 65 and older), black women are more likely to live alone on average (42 percent for Black women, compared to 34 percent for white women) and to face poverty (17 percent for Black women versus 8 percent for white women). Additionally, Black women display the highest rates of self-care disabilities among older women and require more Medicaid assistance (24 percent on average compared to 18 percent for white women).
-
Health Disparities: Mental health issues such as depression and cognitive conditions such as Alzheimer’s disease are more prevalent in older females than older males. Conversely, older males are more vulnerable to life threatening chronic diseases1
like diabetes and cancer. In Central Indiana, older females (age 65 and over) are almost two times more likely on average to have depression (26.2 percent vs 14.5 percent for females versus males) and more likely to have Alzheimer’s disease compared to older males, while older males are more likely to be burdened with diabetes (23.5 percent vs 29.5 percent for females versus males) and to develop cancer.
-
Medicaid Reliance: By the age of 85, approximately 20 percent of women rely on Medicaid assistance, whereas the rate of Medicaid dependency among men remains relatively constant at around 10 percent beyond the age of 65.
-
Nursing Home Reliance: The number of older women residing in nursing homes rises sharply with age, reflecting a greater need for assistance. At the same time, and due to generally more limited financial resources, older women are more likely to rely on Medicaid, public insurance for low-income individuals, to pay for long-term care. In Central Indiana, older women are close to two times (4.7 percent versus 2.8 percent) more likely to reside in a nursing home than men and are increasingly more likely than men to rely on Medicaid for long-term care as they get older.
May 16, 2024 Webinar Recording
Suggested Resources From Webinar
General
State of Aging in Central Indiana Report
Financial Information, SoAR Report Chapter on Financial Stability
Caregiving, SoAR Report Chapter on Caregiving
CICOA Aging & In-Home Solutions
State Health Insurance Assistance Program (SHIP)
Medicare Fraud: Senior Medicare Patrol
Polis Reports on larger issues e.g., improving air quality, water quality, etc. Indiana seems rather low rated on such issues and with little/no research on varying health impacts based on gender
Geriatrics Workforce Enhancement Program (GWEP), University of Southern Indiana
Activities
Young at Heart Dancing Program, Washington Park Family Center
Sassy Seniors Dancing Program– They meet all over the city and once a month they are at The Amp.
Praise Up Gospel Line Dance Ministry
Heritage Place Seniors Programs
Riverside Dance Program, Riverside Parks & Rec Center
Phoenix Theatre Cultural Center senior acting classes and more
Hancock County Senior Services
Ivy Tech Senior Scholars Program
Lawrence Library Fiber Arts Program
Indy Art Center Senior ArtReach Program
Silver Citizens, Inc., Emotional wellness program for older adults
Interesting Reads
Being Mortal, Atul Gawande
Dandelion Wine, Ray Bradbury
Five Invitations, Frank Ostaseki
Our Last Best Act: Planning for the End of Our Lives, Mallory McDuff
Introduction
Indiana, like the rest of the US, is experiencing a surge in its older adult population. The last decade has seen the fastest growth in the age 65 and older demographic compared to any time in the past century.2 As Hoosiers enter old age, we observe long-standing disparities in health and wellbeing between older men and women. While women live longer than men on average, women experience a lower health-related quality of life than do men.3 4 5
Because women have a longer life expectancy than men, they make up a larger proportion of Central Indiana’s aging population. 6 In 2022, there were almost 300,000 older adults aged 65 and older in Central Indiana, 44 percent of whom were men (approximately 120,000) and 56 percent of whom were women (approximately 155,000).
Discussion of male/female disparities and gender inequities is complicated because sex and gender are related but different constructs and are theorized to shape health and wellbeing both independently and interactively.7 Although distinguishing between sex and gender is important for understanding their relative impact on health and wellbeing, the public data sources available for this brief report used only male and female data categories. For readability purposes, this report uses the terms women and men interchangeably with female and male, respectively.
Early Socioeconomic Disparity Affects Women’s Health in Later Life
The economic disparities seen between older men and older women begin much earlier in life. Socioeconomic status, particularly during working years, plays a significant role. Women often face challenges like lower wages 8 and career interruptions due to childcare responsibilities. 9 This translates to lower lifetime earnings and smaller retirement savings compared to men. 10 Because this economic disadvantage persists into their older years, many women are left more vulnerable due to financial insecurity and with less access to quality health care and support for activities of daily living.11
This socioeconomic disparity is evident in Central Indiana, as well.12 While men might experience a sharp income decline only after the age of 85, women are more likely to enter retirement with considerably less and need to stretch those resources further due to their longer lifespans. This creates a situation where some women face financial strain throughout their older years, a burden not shared equally by their male counterparts.
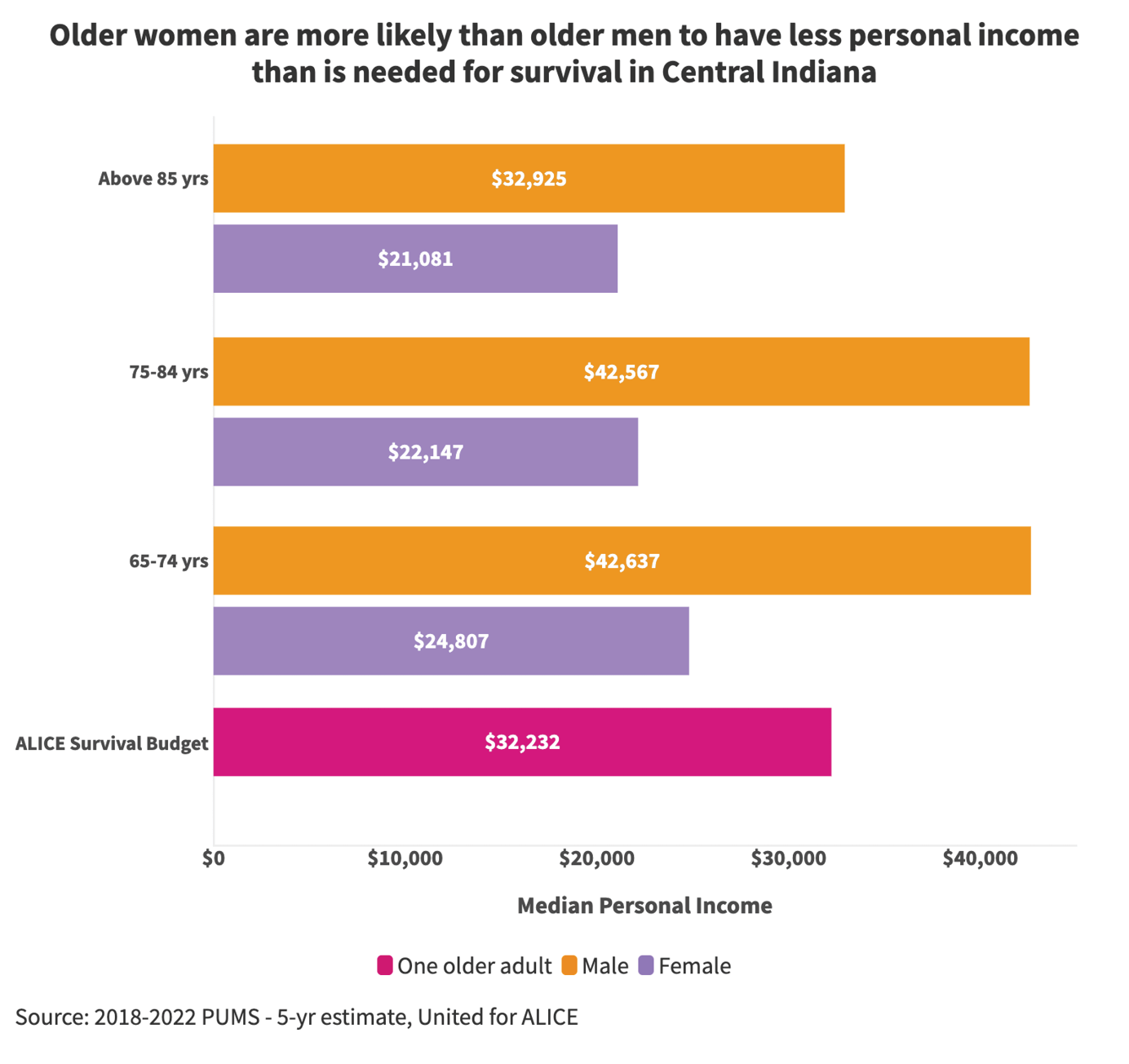
Comparing personal income numbers for older adults with the Asset Limited, Income Constrained, Employed (ALICE) survival budget for Central Indiana further emphasizes the economic vulnerability of older adult women. County-level ALICE survival budgets are based on ten different categories of monthly costs. 13 The total annual survival budget for one senior living alone is $32,232 in Central Indiana. For two older adults living together in Central Indiana, the total annual survival budget is $50,544.
For all older adult age groups, women’s median personal income on average is below the ALICE survival threshold. The personal income of men, on average, does not fall below the ALICE threshold until they are age 85 or older. In Central Indiana, almost 13,000 older adult women live in poverty compared to almost 8,300 older men.
In focusing on just the female older adult population, we see that Black and Hispanic older women start out retirement with significantly less income than their white counterparts.
Many older adults prefer to live independently.14 However, older adults who live alone are approximately 2 time more likely to experience poverty, regardless of sex. Women who live alone are 20 percent more likely to be housing cost burdened than men living alone (49.4 percent versus 41.3 percent for men). In Central Indiana, older women are on average are 70 percent more likely to live alone, with 34.4 percent of older women versus 20.3 percent of older men living alone. Black older women are over 20 percent more likely than white women to live alone (41.6 percent vs 33.7 percent) and almost 90 percent more likely to live alone than Hispanic women (41.6 percent vs. 22.1 percent).
The impact of lower socioeconomic status goes beyond finances. Studies have shown a correlation between lower income and higher rates of depression in older women.15 The financial strain, coupled with potential social isolation and lack of resources, can lead to mental health struggles. Additionally, the gender gap in life expectancy16 means older women often outlive their spouses, potentially facing increased loneliness and a decline in social support networks, further impacting their well-being.17
The next section will explore how these socioeconomic disparities may translate into health outcomes for older women.
Socioeconomic Disparity and the Chronic Disease Burden in Older Adults
Chronic and mental health conditions consume 90 percent of the US’s annual healthcare spending.18
Research has established that gender is an important social determinant of health and that men and women age differently. Disparities such as higher rates of living alone, lower incomes, and higher rates of functional disabilities in older women impact their ability to age well. In turn, men are more likely to be challenged when they lose a spouse, need to act as caregivers, or have to relocate.19 20
In Central Indiana, the average prevalence rates are over 20 percent for diabetes and obesity in both older men and women. When examining male/female disparities, we observe that older men in Central Indiana show a higher prevalence of physical ailments like diabetes (29.5 percent versus 23.5 percent for women) and some cancers, with rates increasing steadily with age.2
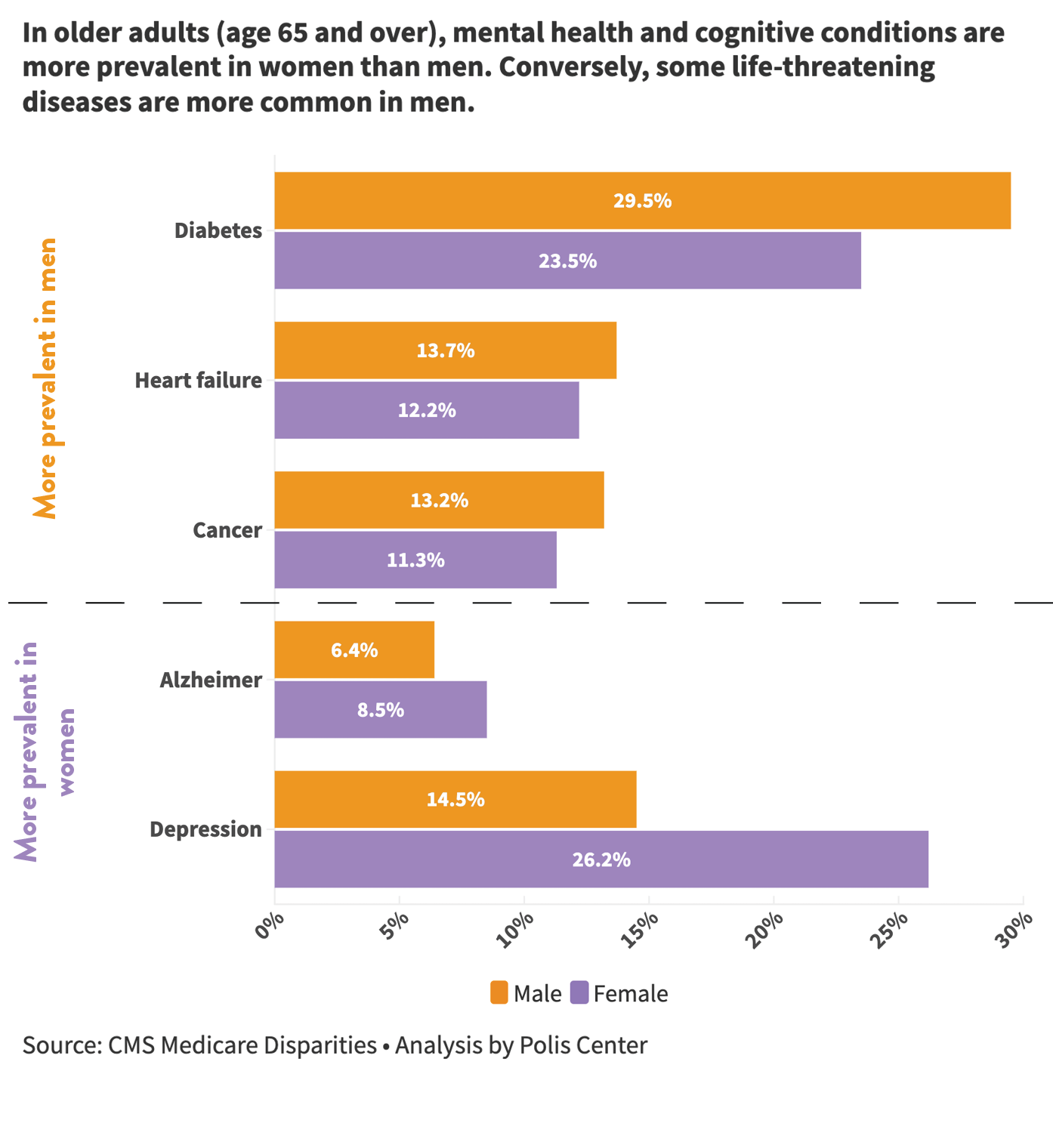
On the other hand, older women face a significantly heavier burden of depression than older men. Central Indiana data show consistently higher rates of depression for older women, mirroring a national trend documented for several years now.15 Higher rates of depression among older women could be influenced by women being more likely to seek mental health care. Research has suggested that only access to healthcare and social limitations predict whether women seek help for self-reported mental health issues, whereas there are numerous sociodemographic and psychological factors that predict whether men seek care.21 However, on average adult women also self-report experiencing more unhealthy mental days than men.
Due to their longer lifespans, women also face an increased risk of developing Alzheimer’s Disease as they age,22 23 which increases their need for long-term care.
In Central Indiana, as of 2022, we have an estimated 95,000 disabled older adults over the age of 65. While having similar rates of overall disability (approximately 34 percent for both sexes), when examining self-care disability rates in particular, we see a pattern emerge that highlights the vulnerabilities of older women as they age. Self-care disability is defined as “a person with a physical, mental, or emotional condition lasting six months or more, who has difficulty in doing any of the activities such as dressing, bathing, or getting around inside the home”.24 In sheer numbers, there are more older women in Central Indiana with self-care disabilities (16,443) compared to older men (7,671).
Self-care disability rates for both men and women increase substantially as they age, with rates for older women rising even more sharply. In Central Indiana, the self-care disability rate for older women increases almost six-fold in post-retirement years (from 5.2 percent in the age 65-74 age range to 29.5 percent in the 85+ age range), compared to older men for whom the rate quadruples (from 4.3 percent in the age 65-74 age range to 17 percent in the 85+ age range).
There are evident racial disparities in self-care disability among older women, with Black women almost two times more likely than white women to be self-care disabled (13.1 percent vs 7.3 percent for white women) and almost one and a half times more likely than Hispanic women to be self-care disabled (13.1 percent vs 8.9 percent for Hispanic women).
Social Isolation and the Fragile Health of Older Women
Social isolation is another threat to the well-being of older adults, particularly women. In the United States, with one in four adults experiencing some form of disability,25 social connections become even more critical for health. While disability rates, discussed above, may be comparable between the sexes, data from Central Indiana paints a concerning picture for older women. Since women live longer and are therefore more likely to live alone once their spouses pass away, they are more likely to face poverty, and struggle with housing costs, especially as they reach their most vulnerable eighties. These factors contribute significantly to social isolation and loneliness, which studies have linked to an increased risk of cardiovascular disease in older women.26
The Need for Improved Access to Long-Term Care
The confluence of social and economic disadvantages creates a complex web of challenges for older women. The increasing longevity of women, particularly those who serve as caregivers for their spouses, coupled with age-related challenges, is contributing to an increased demand for care solutions for older adults. Their need for care intensifies as they age which makes them more likely to rely on institutionalization in nursing homes by their late seventies. This underscores the growing need for health care resources for older adults, particularly women.
While many social determinants of health have been validated as indicators that can explain disparities in health outcomes,27 there is an ongoing need to develop a better understanding of factors that influence the accessibility of services and support needed by vulnerable older adults.
Women are more likely to require Medicaid assistance as they grow older and need nursing home level of care. For the 85+ age group, 20 percent of women are enrolled in Medicaid. Data from the Centers for Medicare & Medicaid Services reveal an uneven distribution of care facilities and service organizations across Central Indiana. Marion County, with its larger population, boasts the highest number of nursing homes and home health agencies. However, quality can vary significantly with only a little over 33 percent of facilities having high quality (four or above) ratings.
Adding to the challenge is the significant cost of long-term care.28 In 2023, the median monthly cost in Indianapolis was $6,000- $7,000 for in-home care, over $6,000 for adult day care, and almost $4,000 for assisted living.29 These costs can leave little room for other essential expenses and potentially push some older adults further into poverty. For patients with moderate dementia and Alzheimer’s, this cost can increase about 20-30 percent.30 Such financial barriers can limit the ability of some older women to access the care they need and impact their overall well-being.
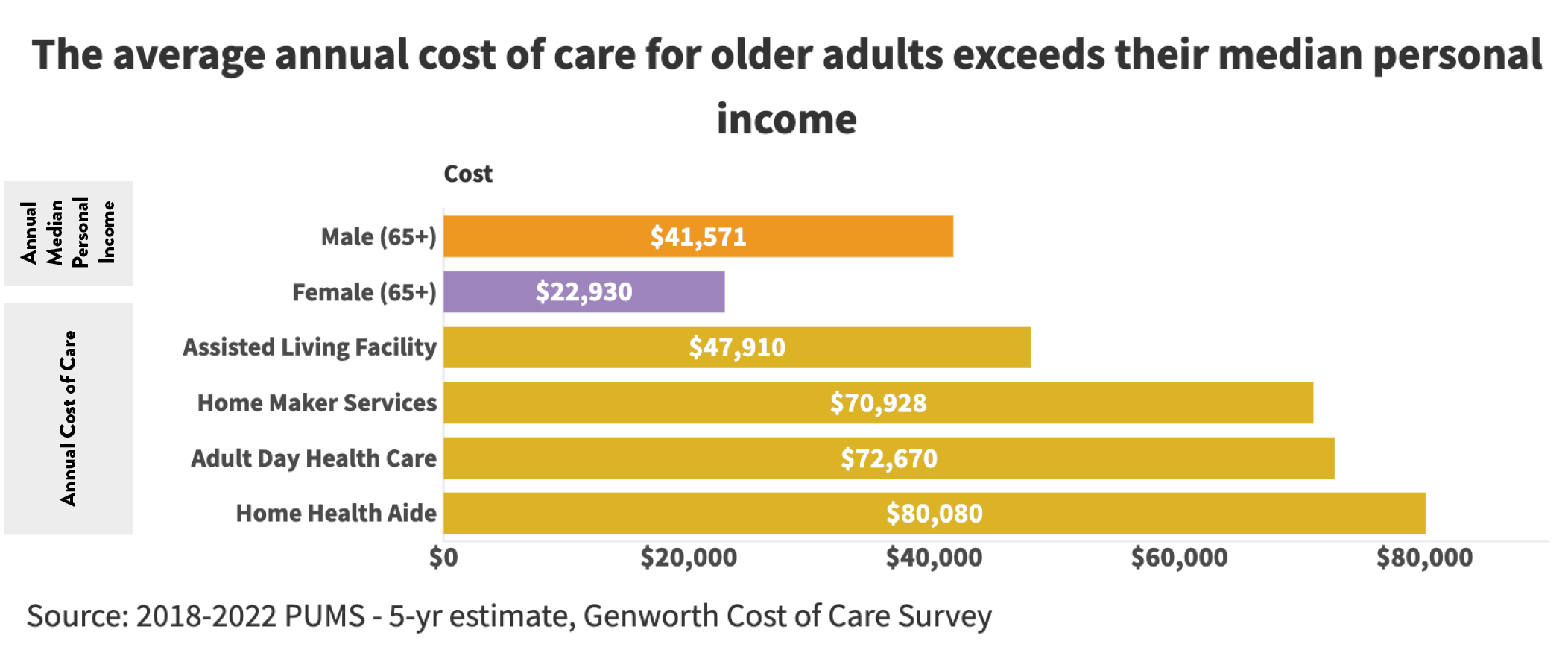
Conclusion
The rising number of financially insecure older women who will need long-term care is a growing challenge in Central Indiana and beyond. Solutions are needed to provide older women with the level of care they need while allowing them to maintain some level of social connection and independence, potentially mitigating the negative health effects of social isolation.
Indiana is attempting to create an improved long-term care system for low-income older Hoosiers by increasing access to community-based and home-based care options.31 In addition to providing affordable and quality options for long-term care, there is also a need to promote increased socioeconomic wellbeing among all older women and equitable access to quality care. The findings in this report raise questions such as:
- As a community, how can we promote equitable access to long-term care and support for our older adult population?
- As individuals, what can women do to improve the likelihood of their being well-cared for in old age?
- Vlassoff, C. Gender Differences in Determinants and Consequences of Health and Illness. J. Health Popul. Nutr. 25, 47–61 (2007).
- U.S. Older Population Grew From 2010 to 2020 at Fastest Rate Since 1880 to 1890. https://www.census.gov/library/stories/2023/05/2020-census-united-states-older-population-grew.html.
- Aging & Socioeconomic Status. https://www.apa.org https://www.apa.org/pi/ses/resources/publications/age.
- Women & Socioeconomic Status. https://www.apa.org https://www.apa.org/pi/ses/resources/publications/women.
- Kaplan, R. M. & Erickson, P. Gender differences in quality-adjusted survival using a Health-Utilities Index. Am. J. Prev. Med. 18, 77–82 (2000).
- Gaps in Life Expectancy Across the Lifespan | The State of Aging in Central Indiana. https://centralindiana.stateofaging.org/2021/09/23/gaps-in-life-expectancy-across-the-lifespan/.
- NIH Office of Research on Women’s Health (ORWH). What are Sex & Gender? And why do they matter in health research? Sex and Gender https://orwh.od.nih.gov/sex-gender.
- Research Summary: Education and Lifetime Earnings. https://www.ssa.gov/policy/docs/research-summaries/education-earnings.html
- Gender pay gap | County Health Rankings & Roadmaps. https://www.countyhealthrankings.org/reports/gender-pay-gap.
- READOUT: US Department of Labor report finds stark gender, age-based pay inequities for older women, whose share of the labor force has increased. DOL https://www.dol.gov/newsroom/releases/wb/wb20230524.
- Cameron, K. A., Song, J., Manheim, L. M. & Dunlop, D. D. Gender Disparities in Health and Healthcare Use Among Older Adults. J. Womens Health 19, 1643–1650 (2010).
- Indiana Income By Gender – 2024 Update | Neilsberg. https://www.neilsberg.com/insights/indiana-income-by-gender/.
- About Us | Overview of ALICE Project. https://www.unitedforalice.org/overview.
- Despite concern about older adults living alone, these seniors prefer the solo life: ‘I love not having to answer to anyone else’. Yahoo Life https://www.yahoo.com/lifestyle/despite-concern-older-adults-living-103027365.html (2024).
- Gueltzow, M., Bijlsma, M. J., van Lenthe, F. J. & Myrskylä, M. The role of labor market inequalities in explaining the gender gap in depression risk among older US adults. Soc. Sci. Med. 332, 116100 (2023).
- Arias, E., Tejada-Vera, B., Murphy, S. L. & Bastian, B. U.S. State Life Tables, 2020. https://www.cdc.gov/nchs/data/nvsr/nvsr71/nvsr71-02.pdf (2022).
- Mohebbi, M. et al. Prevalence of depressive symptoms and its associated factors among healthy community-dwelling older adults living in Australia and the United States. Int. J. Geriatr. Psychiatry 34, 1208–1216 (2019).
- Health and Economic Costs of Chronic Diseases | CDC. https://www.cdc.gov/chronicdisease/about/costs/index.htm (2023).
- Barer, B. M. Men and Women Aging Differently. Int. J. Aging Hum. Dev. 38, 29–40 (1994).
- Matud, M. P., Bethencourt, J. M., Ibáñez, I. & Fortes, D. Gender and psychological well-being in older adults. Int. Psychogeriatr. 32, 1293–1302 (2020).
- Doherty, D. T. & Kartalova-O’Doherty, Y. Gender and self-reported mental health problems: predictors of help-seeking from a general practitioner. Br. J. Health Psychol. 15, 213–228 (2010).
- Alzheimer’s stages: How the disease progresses. Mayo Clinic https://www.mayoclinic.org/diseases-conditions/alzheimers-disease/in-depth/alzheimers-stages/art-20048448.
- Why is dementia different for women? | Alzheimer’s Society. https://www.alzheimers.org.uk/blog/why-dementia-different-women.
- Erickson, W. A. & Lee, C. G. 2007 Disability Status Reports: United States. (2008).
- CDC. Disability Impacts All of Us Infographic | CDC. Centers for Disease Control and Prevention https://www.cdc.gov/ncbddd/disabilityandhealth/infographic-disability-impacts-all.html (2023).
- Golaszewski, N. M. et al. Evaluation of Social Isolation, Loneliness, and Cardiovascular Disease Among Older Women in the US. JAMA Netw. Open 5, e2146461 (2022).
- US DHHS Office of Disease Prevention and Health Promotion. Social Determinants of Health and Older Adults. health.gov https://health.gov/our-work/national-health-initiatives/healthy-aging/social-determinants-health-and-older-adults.
- Indiana Senior Living Communities and Housing. SeniorLiving.org https://www.seniorliving.org/assisted-living/indiana/.
- Genworth Financial, Inc. Cost of Care Survey. Cost of Long Term Care by State | Cost of Care Report https://www.genworth.com/aging-and-you/finances/cost-of-care (2024).
- Paying for Assisted Living & Home Care in Indiana. https://www.payingforseniorcare.com/indiana.
- Zipper, R. Trends in the elder care workforce in Indiana: Evidence for a shift to home-based elder care? https://www.ibrc.indiana.edu/ibr/2022/summer/article1.html.